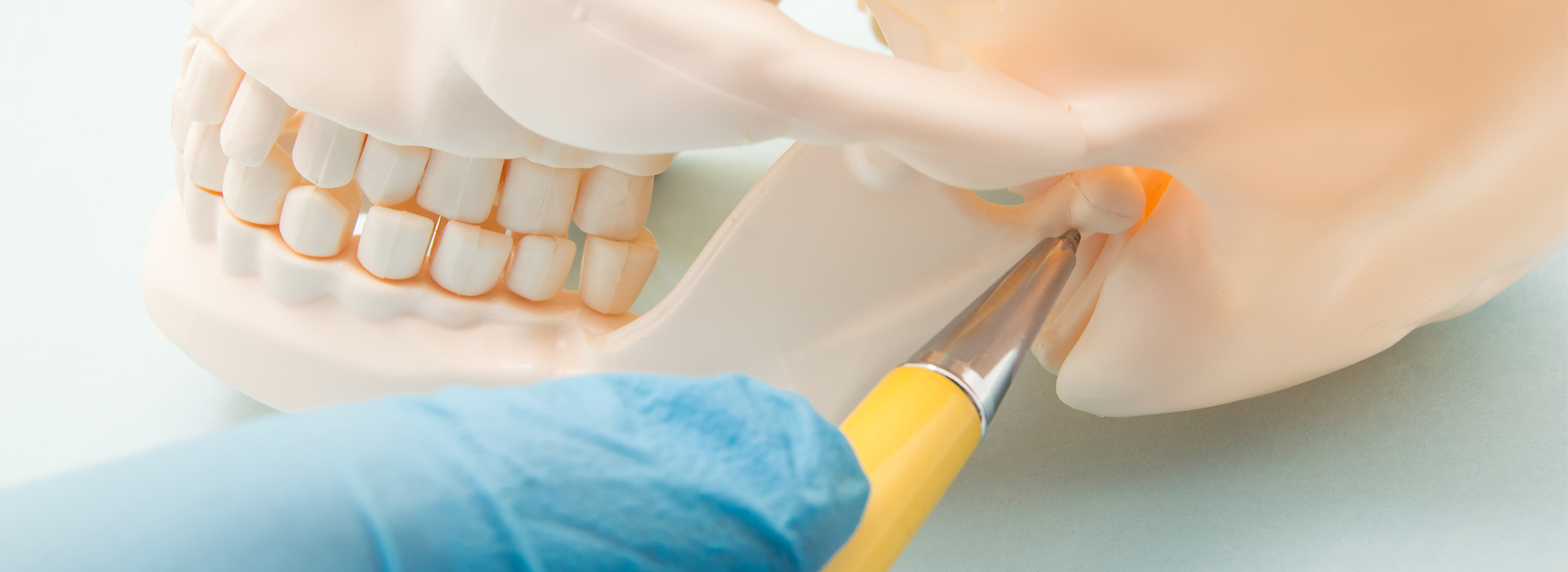
The temporomandibular joint (TMJ) is the hinge and sliding mechanism that links your lower jaw to the skull, enabling chewing, speaking, yawning and the subtle movements that let your face express emotion. Each side of the jaw has its own TMJ, and together they rely on a balance of bone, cartilage, ligaments and muscles to move smoothly. A small, soft disc sits between the moving bones to absorb shock and guide motion, so even minor disruption to that system can produce noticeable symptoms.
Because the TMJ performs both hinge-like and sliding actions, it is one of the most mechanically complex joints in the body. That complexity is part of why disorders of the joint can be hard to diagnose and treat: symptoms can overlap with dental problems, ear conditions, neck dysfunction and generalized facial pain. Understanding the joint and its role in daily function is the first step toward sensible evaluation and effective care.
TMJ disorders affect a significant number of people and are a common cause of chronic facial pain. While many cases respond well to conservative measures, others can become persistent or episodic, impacting sleep, eating and quality of life. Early recognition and a targeted plan help most patients return to comfortable jaw function.
TMJ disorders do not have a single cause; rather, they develop from a mix of mechanical, behavioral and medical influences. Repetitive strain from chronic teeth grinding (bruxism) or clenching is a frequent contributor, as these forces overload the joint and surrounding muscles. Acute trauma — such as a blow to the jaw or an accident — can also damage the disc, ligaments or joint surfaces and trigger ongoing dysfunction.
Systemic conditions that affect joints, including various forms of arthritis, can change the structure and smoothness of the TMJ over time, increasing susceptibility to pain and limited motion. In addition, muscle tension related to stress, poor posture, or neck and shoulder issues can alter how the jaw moves and lead to myofascial pain that mimics or accompanies true joint problems.
Individual anatomy plays a role as well: small differences in tooth alignment, bite relationships, or joint shape can change force distribution and predispose some people to problems. Because multiple factors often interact, a careful history and examination are essential to identify the most likely triggers for each person’s symptoms.
TMJ disorders can present in many ways, and symptoms vary from person to person. Common complaints include persistent jaw pain or tenderness, aching around the ear, clicking or popping sounds during jaw movement, and episodes when the jaw feels stuck or briefly locks. Some patients notice difficulty opening wide, a change in how the upper and lower teeth meet, or increased sensitivity in the muscles that control chewing.
Because the TMJ sits close to the ear and neck, many people experience secondary symptoms such as headaches, ear fullness, ringing in the ear (tinnitus), and neck or shoulder discomfort. These overlapping signs sometimes lead to misdiagnosis, so it’s important to consider TMJ dysfunction when facial or ear-related symptoms persist without an obvious ear problem.
Not all jaw noises or occasional soreness indicate a chronic disorder. However, symptoms that interfere with eating, speaking, sleep, or daily activities — or that last for several weeks despite simple self-care — warrant professional assessment to rule out progressive issues and find the most appropriate interventions.
A thorough clinical assessment is the cornerstone of effective TMJ care. Evaluation begins with a detailed history of symptoms and contributing factors, followed by a focused physical exam of jaw movement, joint sounds, muscle tenderness and bite alignment. The exam also looks for related issues in the neck, shoulders and posture that can influence jaw mechanics.
When needed, imaging studies provide additional information. Panoramic X-rays, cone beam CT scans, or magnetic resonance imaging (MRI) may be ordered to assess bone structure, joint alignment and the condition of the disc. These tests are used selectively and help guide treatment decisions when the clinical picture is unclear or when symptoms persist despite initial therapy.
Because TMJ disorders often benefit from a team approach, a dentist may coordinate care with physical therapists, pain specialists, or medical doctors depending on the findings. This collaborative strategy ensures that treatments address both the joint itself and the muscular or behavioral contributors that sustain symptoms.
Most TMJ problems respond well to conservative, reversible treatments that focus on easing pain, reducing strain, and restoring normal motion. Custom oral appliances such as night guards or stabilization splints are commonly used to protect teeth and decrease nighttime clenching, which allows irritated muscles and joints to recover. Physical therapy and guided jaw exercises can increase mobility, improve muscular balance, and correct postural factors that perpetuate discomfort.
Short-term use of anti-inflammatory medications, targeted muscle relaxants, or therapeutic injections may provide symptom relief in cases where pain is limiting function. In-office interventions are chosen based on the specific diagnosis and are typically combined with self-care measures: a soft-food diet during flare-ups, avoiding extreme jaw movements like wide yawning or prolonged gum chewing, and using warm compresses or cold packs as directed to manage pain and swelling.
When conservative measures fail to control progressive or severe joint damage, more advanced dental procedures or surgical options may be considered. These decisions are made carefully, weighing the potential benefits and risks and often involving specialists when appropriate. Even in complex cases, the goal remains the same: reduce pain, improve function, and help the patient return to comfortable daily activities.
At Capitol Smiles, our focus is on thoughtful evaluation and individualized care for patients with TMJ concerns in Frankfort and the surrounding area. If you’re experiencing persistent jaw pain, recurring jaw noises, or limited motion, a targeted assessment can clarify the cause and outline sensible next steps. Contact us to learn more about how we evaluate and manage TMJ disorders and to discuss which treatment approach may be right for you.
The temporomandibular joint (TMJ) is the hinge and sliding joint that connects the lower jaw to the skull and allows chewing, speaking, yawning and many subtle facial movements. Each side of the jaw has its own TMJ, and smooth function depends on a delicate balance of bone, cartilage, ligaments, a small shock-absorbing disc and the surrounding muscles. Even small disruptions to this system can cause pain, noise or reduced motion that affect daily activities.
Because the TMJ performs both hinge-like and gliding actions, it is one of the most mechanically complex joints in the body and is prone to presenting with overlapping symptoms. Problems in the joint can mimic dental, ear or neck conditions, which is why careful evaluation matters. Early recognition helps guide conservative management and reduces the risk of chronic dysfunction.
TMJ disorders are usually multifactorial and arise from a combination of mechanical, behavioral and medical contributors rather than a single cause. Common influences include chronic teeth grinding or clenching (bruxism), acute trauma to the jaw, degenerative joint conditions such as arthritis, and prolonged muscle tension from stress or poor posture. Small differences in tooth alignment or bite relationships can also change how forces are distributed across the joint, increasing susceptibility in some people.
Because several factors often interact, identifying the dominant triggers for an individual requires a careful history and examination. Addressing only one factor while ignoring others can limit improvement, so a comprehensive approach is usually most effective. Understanding the cause guides the treatment strategy and helps prevent recurrence.
Patients with TMJ disorders commonly report persistent jaw pain or tenderness, aching around the ear, clicking or popping sounds with jaw movement, and episodes when the jaw feels stuck or briefly locks. Many also notice difficulty opening widely, changes in how the upper and lower teeth meet, or increased tiredness in the chewing muscles during the day. Symptoms can vary in intensity and may be constant or episodic.
Because the TMJ lies close to the ear and neck, secondary complaints such as headaches, ear fullness, ringing in the ear (tinnitus) and neck or shoulder discomfort are not uncommon. These overlapping signs can lead to misdiagnosis if the TMJ is not considered, so persistent or function-limiting symptoms should prompt a professional assessment. Occasional jaw noises or minor soreness after vigorous chewing are not always a chronic disorder, but ongoing problems warrant evaluation.
Diagnosis begins with a detailed history and a focused clinical exam of jaw movement, joint sounds, muscle tenderness and bite alignment, along with an assessment of neck and shoulder posture. The clinician will observe opening and closing patterns, palpate muscles of mastication for trigger points, and check for deviations, locking or restricted motion. This hands-on evaluation helps distinguish muscular pain from true joint dysfunction and identifies contributing factors.
Imaging studies are used selectively to clarify the diagnosis when the clinical picture is unclear or symptoms persist despite initial care. Panoramic X-rays, cone-beam CT scans or MRI may be ordered to examine bone structure, joint surfaces and the soft-tissue disc as appropriate. A team approach that may include physical therapy or medical specialists can be helpful when multiple systems are involved.
Most TMJ problems respond well to conservative, reversible treatments that focus on reducing pain and muscular strain while restoring normal motion. Common first-line measures include custom oral appliances such as night guards or stabilization splints to protect teeth and decrease clenching, guided jaw exercises and physical therapy to improve mobility and muscular balance, and posture correction strategies. Self-care techniques such as a soft-food diet during flare-ups, avoiding extreme jaw movements and using warm or cold compresses can also aid recovery.
In cases where symptoms limit function, short-term use of anti-inflammatory medications, targeted muscle relaxants or therapeutic injections may provide additional relief while conservative measures take effect. Treatment plans are individualized and frequently combined to address both the joint and the muscular contributors. The emphasis is on reversible, low-risk interventions before considering irreversible procedures.
Surgical or advanced interventions are generally considered only after a thorough trial of conservative therapies has failed and when objective joint damage, persistent functional impairment or progressive symptoms are documented. Examples include significant degenerative changes, continuing locking that compromises oral function, or a structural problem that cannot be managed nonsurgically. Any recommendation for surgery follows careful evaluation and often consultation with specialists.
When advanced treatment is appropriate, the decision balances potential benefits and risks and is tailored to the patient’s specific diagnosis and goals. Minimally invasive procedures may be attempted before open surgery in some cases, and collaboration with oral and maxillofacial surgeons, pain specialists or rheumatologists can improve outcomes. Clear communication about expected results and follow-up care is an important part of planning.
Dental interventions such as orthodontics, restorative work or occlusal adjustments can sometimes improve how forces are distributed across the jaw and thereby reduce stress on the TMJ. When a clear bite-related contributor exists, correcting alignment or rebuilding tooth contacts may form part of a comprehensive plan to relieve symptoms. However, these irreversible dental procedures should not be the first-line treatment unless a direct causal relationship is established.
Most practitioners prefer to begin with reversible therapies, such as splints and physical therapy, to observe how symptoms respond before proceeding with permanent changes to the bite. If long-term dental or orthodontic treatment is being considered, careful diagnostic records and multidisciplinary consultation help ensure that interventions address the underlying problem. Patient-specific factors and realistic expectations guide the timing and scope of dental treatments.
The TMJ and the muscles that control it share neural pathways with the head, ear and neck, so dysfunction can produce referred pain that presents as headaches, ear fullness, tinnitus or neck and shoulder discomfort. Myofascial trigger points in the chewing muscles can radiate pain to the temples or behind the eyes, and joint inflammation can create sensations that mimic ear disorders. These overlapping patterns are a common reason TMJ problems are initially mistaken for other conditions.
A careful evaluation that considers both dental and medical causes is important when patients present with head, ear or neck complaints. Coordinated care with ENT specialists, neurologists or physical therapists can help pinpoint the source and target treatment appropriately. In many cases, addressing TMJ mechanics and muscular tension reduces secondary symptoms.
Seek professional assessment when jaw pain, persistent clicking, locking episodes, difficulty chewing or changes in how your teeth meet interfere with eating, speaking or sleep, or when symptoms persist for several weeks despite simple self-care. Early evaluation is particularly important if pain is increasing, jaw movement is becoming more restricted, or associated symptoms such as headaches and ear fullness are developing. Prompt attention helps rule out progressive joint problems and identifies effective conservative measures.
A targeted assessment at Capitol Smiles in Frankfort can clarify possible causes and recommend an appropriate, individualized care plan when indicated. Timely diagnosis and a coordinated approach often prevent chronicity and improve long-term function. If you have concerns about jaw pain or related symptoms, scheduling an evaluation sooner rather than later is advisable.
Treatment typically begins with a personalized plan that emphasizes reversible, conservative strategies such as oral appliances, physical therapy, guided exercises and behavioral changes to reduce clenching or bruxism. Providers usually monitor response over weeks to months, adjusting the approach based on symptom improvement and functional gains. Active patient participation in home exercises and ergonomic changes often plays a major role in recovery.
Follow-up care includes periodic reassessment of jaw motion, pain levels and bite relationships to guide any further steps and to determine whether specialist referral is needed. When multidisciplinary collaboration is appropriate, your dental provider will coordinate with physical therapists or medical specialists to address all contributing factors. The goal of ongoing care is to restore comfortable function and prevent recurrence while using the least invasive interventions necessary.
Quick Links